Ambulatory Care Planning: A Quantitative Approach
Ambulatory care has grown dramatically in recent years, and all signs point to continued growth. In 2017 (the most recent year for which data is available), net outpatient service revenue equaled 95% of net inpatient revenue, an increase from 83% in 2013.[1] Clearly every hospital and health system must have an effective ambulatory care strategy.
As providers struggle to keep pace with both traditional competitors and new market entrants (e.g., retail centers), the pressure for rapid implementation of new community-based ambulatory care sites can result in less than adequate planning. This does not need to be the case. With the right information, much of which is readily available, organizations can quickly develop a quantitatively rigorous ambulatory care strategy that addresses the fundamental planning questions: where and what?
A geographic assessment identifies locations that offer the best opportunity for ambulatory care service growth. Even when the region served by an organization is relatively small, it often encompasses wide variation in demographics, socioeconomic status, and competition. It is critical to identify locations that are both attractive and underserved. Once geographic targets are established, market characteristics and organizational strategy can inform selection of specific programs or services, and the appropriate mix of physician specialties to be included in each site.
While numerous qualitative factors are necessary to complete a comprehensive assessment, this article focuses on a quantitative approach to conducting a geographic and programmatic assessment, and prioritization processes.
Geographic Assessment
The first step is to define the specific areas to be examined. Once these are defined, (typically as zip code groupings), they can be evaluated using criteria such as:
- Recent Position: The recent position of the organization within each of the defined sub-regions is the foundation for more detailed analyses. Metrics include inpatient and outpatient market share, and the organization’s existing ambulatory presence in the area.
- Growth Potential: Geographic areas that do not have current strategic value may still have potential for future growth and development, and some current markets may merit service expansion. Look at population projections, land use and development, and emerging employers, as well as proximity to major road systems and public transport.
- Competitive Environment: Effective planning can forestall efforts by competitors in attractive geographic locations. Utilize mapping tools to assess where competitor service locations make them strong or weak, and to highlight gaps in service and areas of opportunity.
- Strategic Fit: Targeted ambulatory services markets must be consistent with and support the organization’s broader strategic plan and other complementary service offerings. They should enhance payer mix, support development of a “destination” service or program, and protect against competitor encroachment.
Programmatic Assessment
Many of the same criteria used to evaluate geographic areas can be used to evaluate programmatic and service line opportunities; the difference will be the specific metrics used. When looking at recent position at a programmatic level, an organization should consider programmatic or service-line-specific indicators. These service-specific considerations (as well as those below) should be applied to the metrics for growth potential, strategic fit, and competitive environment, as well (Figure 1).
Financial Considerations
Programmatic opportunities involve varying financial requirements, recruitment needs, and operational planning. Consider key financial indicators (internal rate of return, contribution margin, downstream revenue potential) when weighing programmatic options.
Ease of Implementation
Physician support generally is the driving force for an initiative’s success, while physician opposition can stop development entirely. It’s essential to have the required operational expertise. In addition to anticipating physician hurdles, an organization must plan for legal, regulatory, and technological barriers to implementation, as well as sufficient budget for staffing, equipping, and marketing.
Figure 1.
Scoring and Evaluation Process
The critical step in the quantitative analysis is assigning a score for each of the metrics. This can be done with a simple scale of one through three, where a “1” represents the lowest opportunity and “3” represents the highest. The scoring for each metric will vary by organization, so it is important to determine appropriate scoring “ranges” for each metric.
For metrics that are qualitative, such as execution difficulty, the evaluators’ perception of low, medium, and high can be scored numerically (in the case of execution difficulty, “3”, “2”, and “1” since low difficulty would mean high opportunity). Specific metrics can be weighted more heavily in the scoring if they are of higher relative importance to the organization, but use weighting with care–it can significantly impact scoring results. Involving key stakeholders when assigning weights to the criteria and metrics prior to scoring can enhance buy-in to final decisions on ambulatory care locations and programs.
Geographic Evaluation
While there may be exceptions, sub-regions that score higher on the geographic evaluation will generally support more robust service offerings.
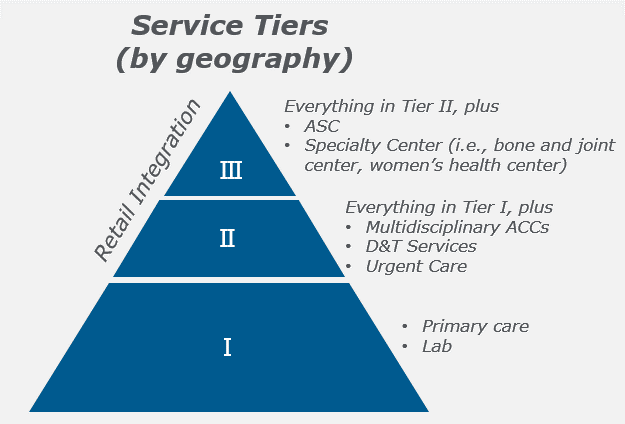
Figure 2 illustrates a sample high-level “tiering” of potential service configurations, to provide a framework for how to think about the scale of service offerings that may be offered across all regions. For example, a region scoring very low on the geographic assessment may only support a minimal incremental primary care presence; a higher scoring region may also support services such as urgent care, surgery, or a specialty center.
Figure 2.
While the geographic assessment identifies the potential service configuration or intensity that each geographic area can support, the programmatic assessment identifies the services that represent the greatest opportunity in each region.
Programmatic or Service Line Evaluation
The key step in the programmatic assessment is to analyze each program or service within the context of each of the regions being evaluated. This is handled similarly to the geographic evaluation, but with the programmatic criteria and metrics scored and weighted. This will identify the sub-regions where a specific program or service has a position of relative strength or weakness. These findings will help determine what offerings are most appropriate within each region and the degree to which they should be developed (See Figure 3).
The Output: Combining Geographic and Programmatic Evaluations
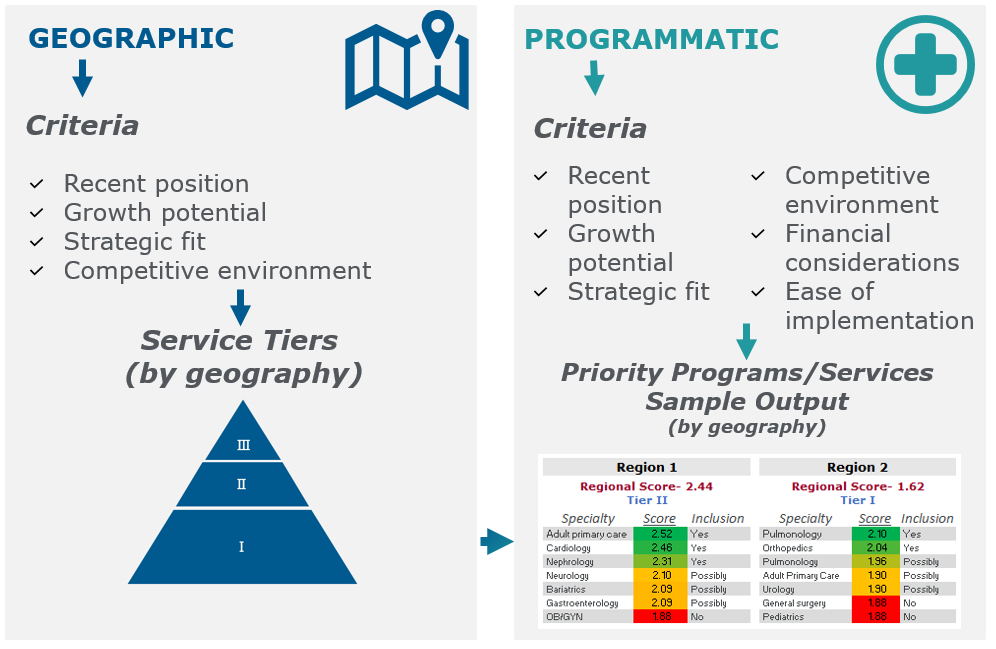
The output of the geographic and programmatic assessments will provide straightforward quantitative results that rank each potential service offering within the context of each region being evaluated. Figure 3 below summarizes the evaluation steps discussed above along with a sample output.
The “art” in this type of analysis lies in translating the scoring of the geographies to specific tiers and the scoring of programs or services to inclusion or exclusion in a particular region. These decisions are best made through facilitation and deliberation.
By accepting this data-driven process, leadership can develop an ambulatory strategy that is timely, thoughtful, and based on solid analysis.
[1]Tara Bannow, “AHA data show hospitals’ outpatient revenue nearing inpatient,” Modern Healthcare, January 3, 2019. At https://www.modernhealthcare.com/article/20190103/TRANSFORMATION02/190109960/aha-data-show-hospitals-outpatient-revenue-nearing-inpatient
Contact the authors:
Craig Holm, Director, cholm@veralon.com
Scott Stuecher, Manager, sstuecher@veralon.com