Systemness: The Next Frontier for Integrated Health Delivery
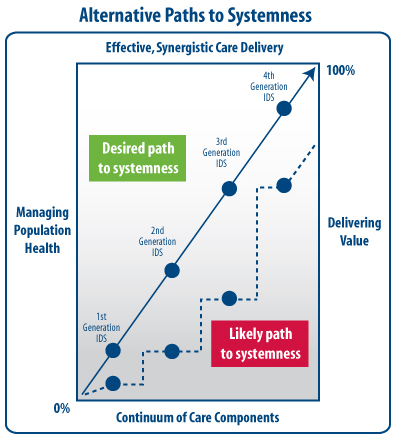
Systemness is a term increasingly used to describe the desired future state of complex health care delivery systems, which will deliver patient-focused, seamless, and high-quality care across the many components of the system to maximize value for customers. Some integrated delivery systems are still first generation enterprises, as noted in the exhibits below, and have not progressed far in functioning as a synergistic entity. Others have begun the journey to third and fourth generation organizations.
Systemness Priorities
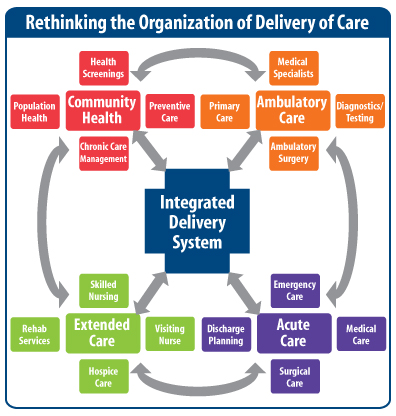
For most organizations, the path to systemness focuses first on assembling the needed system components and rebalancing, as necessary, the system’s scope and scale as shown in the exhibit below. Many first and second generation systems are still making the shift from a hospital- and ambulatory-centric enterprise to the full, balanced continuum of care. This shift involves developing, directly or through partnerships, the full and appropriately sized range of extended care and community health resources and starting to integrate them with other system services. It may also involve a rethinking of the integrative mechanisms for care from those that are more virtual to the extensive use of medical homes as an integration hub.
As the path to systemness advances, the focus moves toward maximizing the effectiveness of clinical operations. This initiative involves optimization of quality/safety and patient satisfaction, initially at the unit/episode of care level and then for programs and patient populations. Reducing variation and eliminating waste are key themes during this stage.
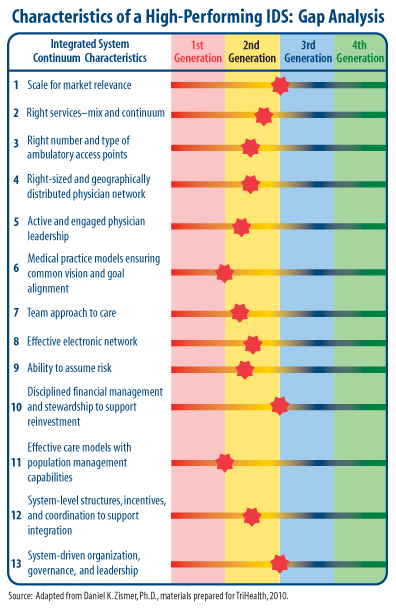
The migration to systemness moves to a higher level as the focus shifts to value, with cost/price to customer explicitly considered along with the care delivery process, and ultimately the health of populations. Many of the factors involved in creating a high-performing integrated delivery system and moving up the continuum from first to fourth generation are illustrated in the exhibit below. Characteristics 1-4 have largely been addressed above. Characteristics 5-7 deal with the alignment and leadership of physicians and medical practices and the clinical teamwork necessary in advanced care delivery models. This is facilitated by characteristic 8, IT infrastructure, which also helps to support the ability to assume financial risk, achieve advanced financial management, and migrate to sophisticated care delivery models. Finally, the last five characteristics involve required organizational structures, systems, and processes to support the enterprise.
Systemness and the move to the highest level of integrated delivery system performance is characterized by a long-term commitment to developing a continuum of care in an effective synergistic care delivery model, which maximizes customer value and addresses proactively the health of populations. While the journey to systemness may vary, the likely path for many organizations and key considerations to progress there follows the linear and step function from first to fourth generation, with a few variances along the way.