Moving Beyond Large Group Practice Acquisition to Successful Operation
Strategies & Solutions
2013
Larger physician practices, both primary care and specialists, are increasingly the focus of hospital and health system acquisition efforts. If a large practice is not affiliated with the buying organization, or if it refers a relatively small percentage of their clinical business to them, acquisition of the practice can generate significant incremental volume and improve market position. For physician practices, acquisition provides a buffer from the risks and pressures that make running a successful practice an increasingly challenging task in an era of health care reform and changing reimbursement practices.
Large physician practices are particularly well suited for the acquisition process, as they can leverage their size and referral power at the bargaining table. Recent data released by Irving Levin Associates report that the overall dollar value of large group practice acquisitions increased substantially from 2011 to 2012. Although transaction details for physician practice acquisitions are rarely made public, on average, a practice with more physicians will generally sell at a higher price per FTE physician than a practice with fewer physicians.
Focusing on Priorities
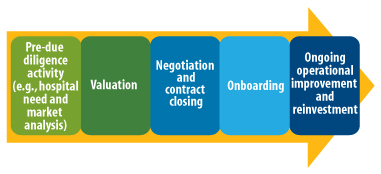
As hospitals and health systems scramble to acquire these large practices in an offensive or defensive market strategy, hospital administrators and business development teams often view the transaction closing date as the finish line. Prudent health care leaders recognize that to capitalize on the significant practice investment, a comprehensive integration strategy, from pre-due diligence through onboarding and beyond, must be employed and successfully executed, as illustrated below.
Physician Practice Acquisition Continuum
While effective planning and diligence are required in all areas of this continuum, the onboarding process is often the phase that has the greatest potential to set the stage for smooth integration and acceptable returns on investment.
Medical practice executives and physicians cite the following aspects of the onboarding process as the most influential on overall success:
- Start early. A typical practice transition process should start at least 60 days prior to the transaction closing date; best practice onboarding process begins 90 days prior to practice start date.
- Concentrate on culture. A large practice will come with its own history and unique culture; do not let this deter your organization from sharing its own cultural components that will most heavily impact the practice’s ability to assimilate with the rest of the organization. Staff should attend health system orientation, patient satisfaction training, have access to leadership development programs, and receive public acknowledgement as new members of the health system team. These cultural components often have a significant influence on overall practice satisfaction with the transition.
- Implement hospital IT and other systems from the outset. Large practices often have different IT systems than the acquiring system, or even home-grown software programs, including electronic medical records and billing/coding systems; health systems may be tempted to allow groups to keep their current system(s) in the transition or permanently. This leads to costly (and lingering) interface and operational issues.
- Identify patient flow and referral patterns. Understand, from the patient perspective, a clear process flow within the office and potential transitions to and from the hospital, physician specialists, and/or other ancillary/outpatient settings. This step will make the transition process seamless to patients and may also identify and eliminate operational inconsistencies.
- Over communicate. Hold regular staff, physician, and leadership meetings to engage the new practice on progress and discuss/resolve issues that arise, and ensure that other medical staff members and hospital leadership are aware of the new clinical resources. Hospital and physician leaders say that a majority of transition issues result from a lack of communication before and during the process.
Keys to Ongoing Success: Operational Performance
Successfully integrated physician networks require ongoing support following onboarding to improve operational performance. Below are steps to consider when planning for the future viability of employed physician practices:
- Explicit contracts. Make employment contracts explicit regarding expectations and performance incentives with limited terms (e.g., one to three years)
- Regular feedback. Provide regular feedback and data to employed physicians on productivity, quality measures, revenue generation, expense levels, overall operations, and other practice performance measures
- Focus on efficiency. Centralize larger administrative functions (e.g., billing and collections), to achieve economies of scale and scope and permit physicians to focus on day-to-day operations of the practice
- Set limits for losses/subsidies.Establish guidelines for the per-physician operating loss or subsidy that will be tolerated
- Evaluate and adapt. Conduct ongoing evaluations of employment relationships to identify if changes in the practice or regulatory environment warrant a change in the employment relationship
Through consideration of these strategic issues, coupled with efficient operational and financial integration of processes, a practice will be more likely to achieve its projected volume and revenue targets within the first year, and be well positioned for future success as a vital member of the acquiring organization.